|
View the:
Paper (author's version)
Paper (JVIR)
|
Boas FE, Do B, Louie JD, Kothary N, Hwang GL, Kuo WT, Hovsepian DM, Kantrowitz M, Sze DY. (2015) "Optimal imaging surveillance schedules after liver-directed therapy for hepatocellular carcinoma." J Vasc Interv Radiol. 26(1):69-73.
Abstract
Purpose: To optimize surveillance schedules for detecting recurrent hepatocellular carcinoma (HCC) after liver-directed therapy.
Materials and Methods: New methods have emerged that allow quantitative analysis and optimization of surveillance schedules for diseases with substantial rates of recurrence such as HCC. We applied these methods to 1766 consecutive chemoembolization (TACE), radioembolization (RE), and radiofrequency ablation (RFA) procedures performed on 910 patients between 2006 and 2011. The CT or MRI obtained just prior to repeat therapy was set as the time of recurrence. "Recurrence" included residual and locally recurrent tumor, as well as new liver tumors. Time-to-recurrence distribution was estimated using Kaplan-Meier. Average diagnostic delay (time between recurrence and detection) was calculated for each proposed surveillance schedule, using the time-to-recurrence distribution. An optimized surveillance schedule could then be derived to minimize the average diagnostic delay.
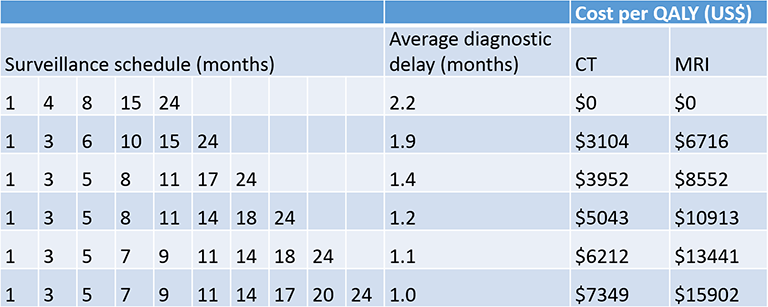
Results: Recurrence is 6.5 times more likely in the first year after treatment, compared to the second. Therefore, screening should be much more frequent in the first year. For 8 time points in the first 2 years of follow-up, the optimal schedule is 2, 4, 6, 8, 11, 14, 18, and 24 months. This schedule reduces diagnostic delay compared to published schedules, and is cost effective.
Conclusion: The calculated optimal surveillance schedules include shorter interval follow-up when there is a higher probability of recurrence, and longer interval follow-up when there is a lower probability. Cost can be optimized for a specified acceptable diagnostic delay, or diagnostic delay can be optimized within a specified acceptable cost.
Keywords: surveillance, hepatocellular carcinoma, transarterial chemoembolization, radioembolization, radiofrequency ablation
|